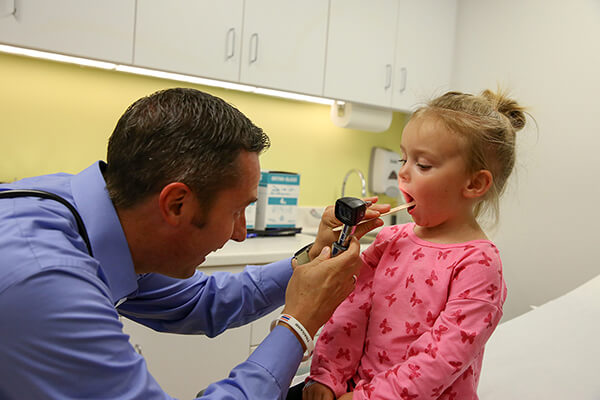
Last week we discussed bronchiolitis, which is usually caused by RSV. Today I want to help you better understand croup. Croup is swelling of the upper airway caused by a virus, usually Parainfluenza. Despite the name, Parainfluenza has nothing to do with Influenza.
Parainfluenza circulates in Utah any time it feels like it and makes children’s tracheas swollen, which earns it a place on pediatricians’ “virus enemies” list. It usually affects older infants, toddlers, and young children. Little children’s tracheas are usually narrow and floppy, so even a little bit of swelling around on the inside can make it very difficult to breathe.*
The symptoms of croup include barking cough and stridor (which I will explain) that are worse at night,** and fever. Usually, the second night is the worst night of croup, then it gradually turns into a normal cold that can linger for 1-2 weeks. The child is contagious for 2-3 weeks, but other children with the same virus might be contagious with croup but not have croup symptoms. By barking cough, I mean it sounds like a seal barking. Click the link to hear a barking cough:
By stridor, I mean a tight or squeaky sound when the child is breathing in. This is different from wheezing, which is a multiple-whistling sound when you breathe out. Here is what stridor sounds like:
When should my child see the pediatrician for Croup?
Come in for stridor, working hard to breathe, or under-immunized status. Further explanation follows:
If your child has barking cough without stridor, you can probably manage this at home with close observation, increased fluids, and breathing cold air outside. However, children who have stridor (even if it’s only at night) should see the pediatrician. If the stridor is only with crying, then you can wait until daytime to be seen. However, if there is stridor with labored breathing when at rest (not just with crying), that is not relieved right away by breathing cold air outside, then go to the emergency department. If your child has difficulty breathing with retractions (a “sucking in” of the skin above, below, and between the ribs or at the bottom of the neck when breathing in), then seek immediate medical attention at the office or ER. Children who are behind on immunizations (especially the Hib – Haemophilus vaccine***) should go to the ER or their pediatrician right away if they have stridor or difficulty breathing – and be sure to remind the doctor that your child has not had all the shots. If a child has a high fever (over 102) and is leaning forward and drooling, this can be a sign of bacterial infection of the trachea or epiglottis (the flap that can cover and plug up the top of the trachea) which can be life-threatening. Also, see your pediatrician if you think the stridor might be caused by something else (like an object or food that got stuck in the trachea, or a baby who has had “stridor since birth” who might have an abnormality of the airway).
What is the treatment for croup?
The two best treatments for croup are breathing cold air and a single dose of anti-inflammatory steroids (injected or by mouth). High-concentration humidity with a cool air humidifier right in front of the child for 10 minutes, can also help. If the croup is mild, the steroid helps but is not mandatory. Moderate to severe croup usually is treated with the steroid. At night, if your baby has stridor, bundle him up and take him outside to breathe cold air. The cold air molecules touch the inside of the trachea and can help decrease the swelling. In the office or emergency department, if the croup is severe, we sometimes give nebulized adrenaline (epinephrine), which can decrease the trachea swelling for a couple of hours while we wait for the steroid to start working. This medicine is generally not prescribed for home use. If the treatments are not working, or if the stridor is significant during the day, then she might need to be admitted to the hospital, usually for a couple of nights, until the tracheal swelling decreases.
I hope you feel more empowered to take care of your child with croup. Your pediatrician is ready to help you through it if you are concerned.
Payson and Spanish Fork, Utah, USA
Footnote factoids — some croup questions that curious parents sometimes ask, and nerdy doctors love to answer:
* Why do children get croup and not adults? A child with a trachea narrowed from croup is often miserable because it’s hard for her to breathe in. An infant’s trachea is sometimes only about 4 millimeters in diameter. If it’s swollen only a little, say 1 mm all the way around the inside, then that shrinks the diameter to 2 millimeters. The flow rate of air through a pipe is proportional to the fourth power of the diameter of the pipe. So, if a baby’s trachea is half its normal diameter, then only 6{81e69a3ca26977ac766aed87a28b2a1ecd92f9787a94c83a7ea2b436f670aee6} of the normal air can get in. If the baby is crying, it’s even worse. With the turbulent airflow during crying, the flow of air is proportional to the 5th power of the diameter, giving the croupy baby only 3{81e69a3ca26977ac766aed87a28b2a1ecd92f9787a94c83a7ea2b436f670aee6} of the normal airflow. If an adult with a 16mm trachea gets the same virus, and his trachea has the same 1mm swelling so that it narrows from to 14mm, it’s not such a big deal, because air can get in at 88{81e69a3ca26977ac766aed87a28b2a1ecd92f9787a94c83a7ea2b436f670aee6} of the normal adult flow rate (14/16)^4.
** Why is croup worse at night? Croup is worse at night for two main reasons: the muscles in the neck and throat that hold open the airway in the day are more relaxed at night, and our body’s adrenal glands make more natural corticosteroids during the daytime hours, which partially treat the croup in the daytime. Often, when I see toddlers in the office on a morning after a stressful night of croup with seal-barking cough and stridor, they are not doing it anymore for me because it’s daytime. The parents and I sometimes resort to dramatic reenactments and listening to recordings of croup cough and stridor to describe well what was just happening last night at home. Without treatment, the second night is usually worse than the first night.
*** I am so glad I’m a doctor in this century and not the last one! Before Hib vaccine became available in the late 1980s, a more severe and life-threatening form of bacterial croup, caused by Haemophilus B, was more common. The bacterial versions of croup (also called bacterial tracheitis and epiglottitis) were so much worse than viral croup, that in the old days viral croup was called “faux croup” and the bacterial croup was just called croup. Thanks to Hib, epiglottitis and bacterial tracheitis caused by Haemophilus are rarer. I have only seen it twice, both in children whose parents had refused immunization. Both were hospitalized, their windpipes became blocked almost completely, and they nearly died. Some older doctors I know have stories of kids dying from Haemophilus bacteria before we had Hib vaccine. If we keep our children immunized, then Haemophilus B epiglottitis and tracheitis (along with meningitis also caused by Haemophilus) won’t come roaring back to Utah.