Chances are you know someone who has been affected by breast cancer. For one out of every eight women, the risk of being diagnosed with it is relatively high. Hereditary breast cancers are only responsible for 5 to 10 percent of breast cancer cases. However, there is a significantly higher risk for women who have the BRCA1 BRCA2 genetic markers.

Epigenetics is the study of how the environment and your behaviors can affect gene expression. The DNA sequence is not altered, but epigenetic changes affect how the body reads your DNA and determines health outcomes.
Consulting with a genetic counselor or doing a genetic screening test is beneficial for at-risk individuals. These women have a family history that includes one of the conditions below.
One (or more) first– or second-degree relative(s) with:
- Breast cancer diagnosed at age 45 or younger in women
- Triple-negative breast cancer diagnosed at age 60 or younger in women
- Primary cancer of both breasts
- Both breast and ovarian cancer in the same relative
- Male breast cancer
- Ovarian cancer
- Two or more first– or second-degree relatives from the same side of the family with breast cancer, if at least one breast cancer was diagnosed before age 50.
- Three or more first– or second-degree relatives from the same side of the family with breast or high-grade prostate cancer at any age.
- Ashkenazi Jew Ancestry

BRCA1 and BRCA2 are examples of epigenetic changes that have significant consequences. BRCA genes are tumor suppressor genes that help combat breast cancer by making proteins to repair damaged DNA. These tumor-suppressing genes do not work correctly for women who have the BRCA1 or BRCA2 genetic marker. These women should be counseled appropriately regarding increased breast surveillance (clinical examinations and imaging/mammograms), starting a family, and possibly undergoing prophylactic surgery to decrease the risk of breast cancer.

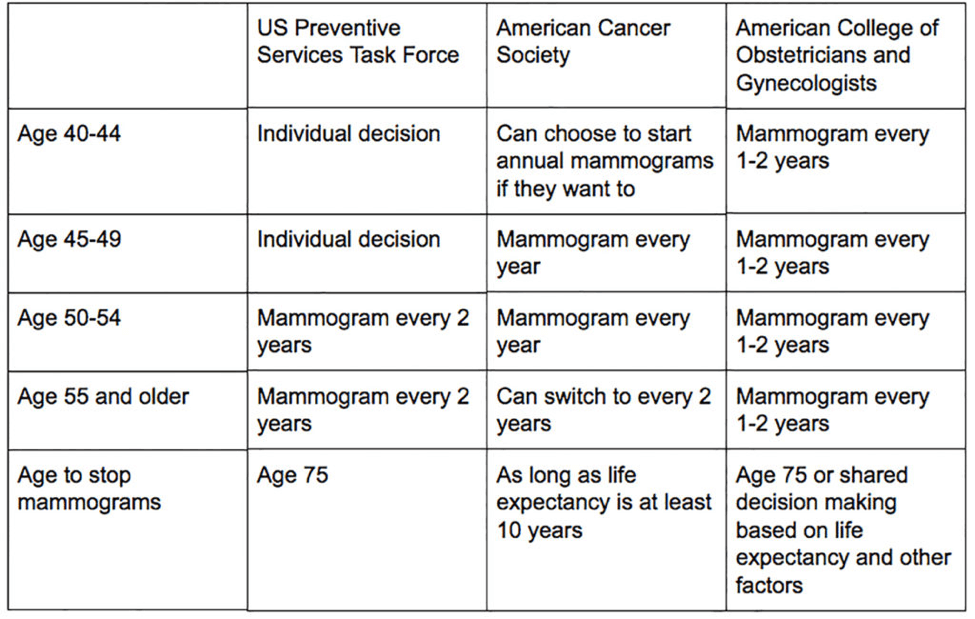
Talk to your provider about your family history and potential genetic risk. Do not be fearful, be hopeful. Breast cancer is very treatable, mainly when it is discovered early and treated appropriately. On average, mammograms detect cancer two to three years before a lump is felt. Mammograms are usually covered 100 percent by insurance companies, and there is no copay on your part. If you do not have the means to have a screening mammogram done, contact the Utah County Health Department, as they may help cover the cost of this service. Please complete routine screening examinations and mammograms as recommended for your age and level of risk.
References
American Cancer Society (ACS). (2019). Breast cancer survival rates. https://www.cancer.org/cancer/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-survival-rates.html
American Cancer Society (ACS). (2019). Breast cancer risk factors you cannot change. https://www.cancer.org/cancer/breast-cancer/risk-and-prevention/breast-cancer-risk-factors-you-cannot-change.html
Centers for Disease Control and Prevention (CDC). (2020). What is epigenetics? https://www.cdc.gov/genomics/disease/epigenetics.htm
Dullens, B., de Putter, R., Lambertini, M., Toss, A., Han, S., Van Nieuwenhuysen, E., Van Gorp, T., Vanderstichele, A., Van Ongeval, C., Keupers, M., Prevos, R., Celis, V., Dekervel, J., Everaerts, W., Wildiers, H., Nevelsteen, I., Neven, P., Timmerman, D., Smeets, A., Denayer, E., … Punie, K. (2020). Cancer Surveillance in Healthy Carriers of Germline Pathogenic Variants in BRCA1/2: A Review of Secondary Prevention Guidelines. Journal of oncology, 2020, 9873954. https://doi.org/10.1155/2020/9873954
National Breast Cancer Foundation (NBCF). (2021). BRCA: The breast cancer gene. https://www.nationalbreastcancer.org/what-is-brca
U.S. Preventive Services Task Force (USPSTF). (2019, August 20). BRCA-related cancer: Risk assessment, genetic counseling, and genetic testing. https://www.uspreventiveservicestaskforce.org/uspstf/recommendation/brca-related-cancer-risk-assessment-genetic-counseling-and-genetic-testing