Did you know November is National Diabetes Month? This year’s theme is prediabetes. Let’s celebrate by learning more about prediabetes and what we can do to improve our health!

What is prediabetes?
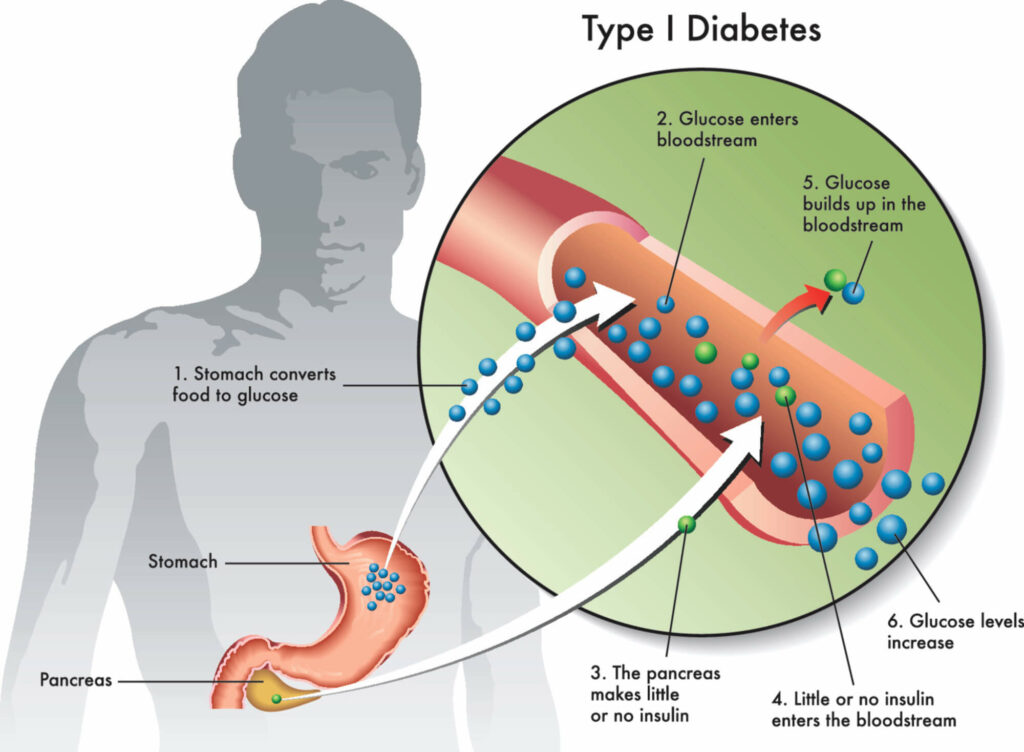
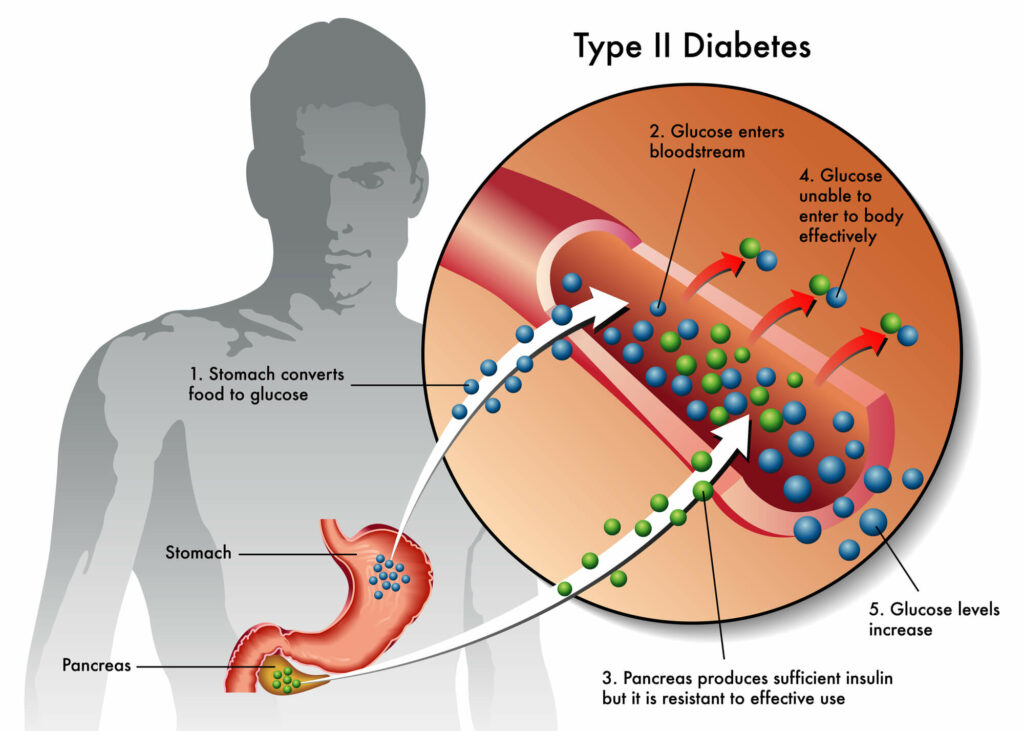
In prediabetes, your body doesn’t use insulin well. Insulin helps the cells in your body use sugar for energy. If your body doesn’t use insulin well, the sugar stays in your bloodstream, and your blood sugar rises. Prediabetes causes higher than normal blood sugar levels, but not high enough to be type 2 diabetes. Too much sugar in your blood can lead to serious long-term problems for your eyes, kidneys, heart, and brain. I don’t like the sound of that, so how do you know if you have prediabetes? Let’s find out.

How do I know if I have prediabetes?
More than 1 in 3 people in the US have prediabetes, and more than 84% of them don’t know it! There are often no signs or symptoms of prediabetes. Many people have it and don’t even know they are at risk for serious health problems. Is there some good news here? Yes! A simple blood test can tell us if you have prediabetes.
Certain people are at higher risk. It’s important to know if you are at higher risk to discuss with your healthcare provider and find ways to lower your risk. Risk factors for prediabetes include:
- Being 45 years or older.
- Being overweight.
- Having a parent or sibling with type 2 diabetes.
- Not being physically active.
- Ever having gestational diabetes.
- Having polycystic ovary syndrome.
African Americans, Hispanic/Latino Americans, American Indians, and Pacific Islanders are also at increased risk.
The CDC has an online test you can take to help you determine your risk can find it at this link: https://www.cdc.gov/prediabetes/risktest/
Do you want more good news? If you know you have prediabetes, there are many things you can do to prevent long-term complications, including type 2 diabetes. You can even reverse prediabetes!

How can I reverse prediabetes and prevent type 2 diabetes?
Start small! You don’t have to do all of these all at once. Making lifestyle changes is hard. Small, manageable goals are more sustainable. Get support from your friends and family. Remember, you can start small, and you can start today- don’t wait for the new year for new goals!
- See your healthcare provider: A simple blood test can be done to check for prediabetes and diabetes. Remember, there are often no symptoms or signs of prediabetes, so regular checkups with your healthcare provider and discuss your risks are essential! Make an appointment today.
- Exercise: It’s okay to start small. Try to find something you enjoy doing and do it with people you enjoy spending time with. The goal is 30 minutes of exercise 5 days per week.
- Healthy diet: Choose foods that are lower in fat and sugar. Try to balance your plate with vegetables, lean protein, and grains. Avoid sweetened beverages and drink more water.
- Lose weight: A small amount of weight can make a big difference! Losing just 5-7% of your body weight can lower your risk of getting type 2 diabetes.
- Quit Smoking: If you smoke, consider quitting. Get help quitting by talking to your healthcare provider. If you don’t smoke, don’t start.
- Stay up to date on vaccinations: This may not prevent prediabetes, but it can prevent serious complications if you get sick with a vaccine-preventable illness like the flu or COVID-19. Come in to get updated on your vaccines today!

Happy National Diabetes Month! Pick one of these steps to start this November to celebrate!
References
Center for Disease Control and Prevention. (2020). Prediabetes- Your chance to prevent type 2 diabetes. https://www.cdc.gov/diabetes/basics/prediabetes.html
National Institute of Diabetes and Digestive and Kidney Diseases. (2021). National Diabetes Month 2021. https://www.niddk.nih.gov/health-information/community-health-outreach/national-diabetes-month
Resources
https://www.cdc.gov/diabetes/prevention/index.html
https://www.cdc.gov/diabetes/index.html
https://www.niddk.nih.gov/health-information/diabetes/overview/preventing-type-2-diabetes/game-plan