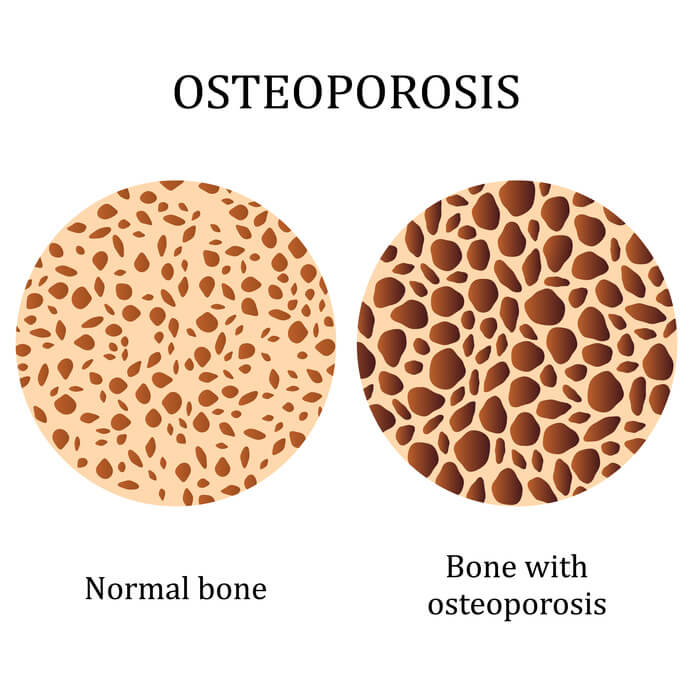
May is National Osteoporosis Awareness and Prevention Month! This is a great time to pause and think about the health of one body system we sometimes take for granted: the skeleton!

The human body has 206 bones, and they are made up of active, living tissue. The health and wellbeing of your skeletal system is critical for getting you around to live your life, but we often don’t think about it until a bone breaks. Children and adolescents tend to have stronger bones made of cells that regenerate at much higher rates. By about age 30, our bone mass peaks and slowly decreases for the rest of our lives.
In addition to this bone mass loss that is a normal part of aging, some adults may develop a disease called osteoporosis. The disease results in excessive loss of bone density, causing the bones to become weak and brittle. It is sometimes called “the silent disease” because there are often no symptoms until a bone fractures. It is different from osteoarthritis, which is a painful joint disease. At least one in two women and one in four men over age 50 will break a bone at some point due to osteoporosis. This disease can cause pain, suffering, and loss of mobility if it progresses too far. Luckily, osteoporosis can be treated and even prevented!

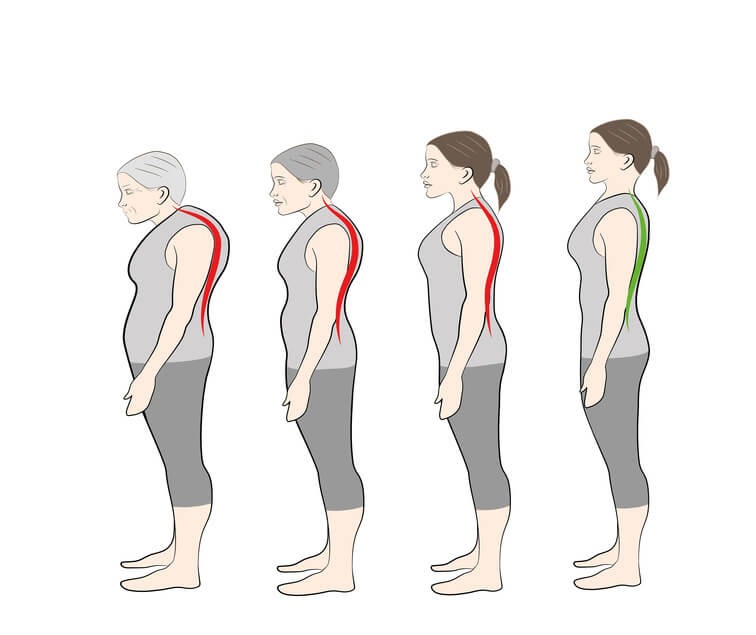
Preventing osteoporosis is a topic near and dear to my heart – not just because as an OB/GYN PA I am keenly aware of how it disproportionately affects women, but also because my own grandmother suffered from osteoporosis. I watched her lose several inches of height as the disease caused her posture to become more and more stooped over time. Luckily, my grandma never broke any bones, but we were always worried about the potential of a life-altering injury if she had a fall. Because of my grandma’s experience with osteoporosis, my mom is keeping a careful eye on her bone health, and I am too. The best ways to prevent osteoporosis are to make healthy lifestyle changes and talk with your healthcare provider about appropriate screenings.
Everyone knows that we should eat a healthy diet and get regular exercise, but you may not know that these good habits can make you less likely to have bone problems when you are older. Since I am getting closer to the age where my bones will stop replacing themselves as well, I make sure to get plenty of calcium and vitamin D in my diet. These are the nutrients your body needs to build bone. You can get calcium through milk and dairy products, but also from things like leafy green vegetables, fortified breads and cereals, and supplements if necessary. For more information about how much calcium and vitamin D you need and how to get it, see the FDA website on recommended daily intake or talk to your healthcare provider.
My mom watches her diet, goes on daily walks, and plans to get a DEXA scan when she turns 65. A DEXA scan is a type of X-ray where we can measure how dense your bones are. If this testing shows that you are at increased risk for fractures, there are medications we can use to help build up your bones. All women 65 and older should have a DEXA scan, as well as anyone at increased risk of low bone density, which may include people with a history of long-term steroid use or a family history of osteoporosis.

No matter what stage of life you are in, you can make changes to improve your bone health. It’s so important I’ll say it one more time: make sure you are getting enough calcium! And don’t forget vitamin D. Live an active life and do some kind of weight-bearing exercise (like walking, running, aerobics, or resistance training) regularly to help keep your bones strong. Avoiding smoking and minimizing alcohol intake can also decrease your risk of developing osteoporosis. Stay up to date on regular health screenings including your DEXA scan if applicable. If you have been diagnosed with osteoporosis, make sure you have a plan for preventing falls. And as always, personalized medical advice is the best kind of advice, so talk to your healthcare provider about how to keep your skeleton healthy.
For more information, please see:
Blogs from Kristen Wright, FNP – https://canyonviewmedical.com/news-blog/going-break-hip-bone-health-part/
National Osteoporosis Foundation – nof.org